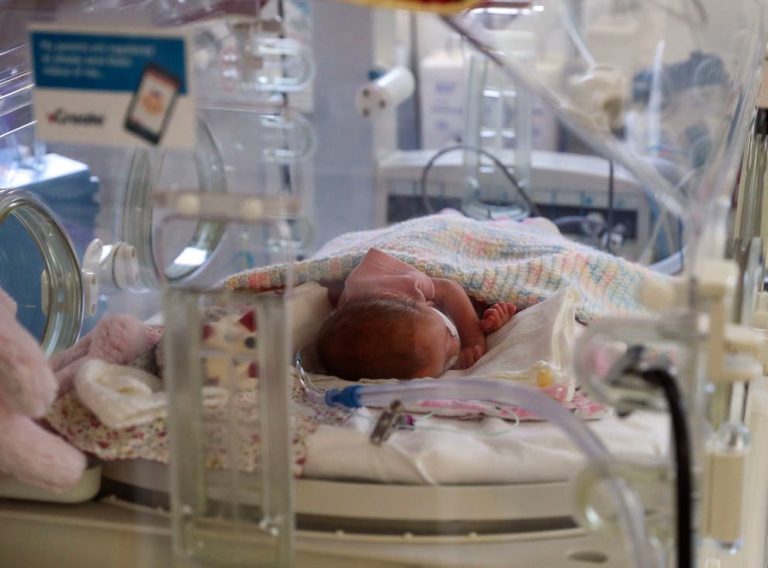
Shrewsbury and Telford Hospital Trust has been blamed for the deaths of more than a dozen mothers and more than 40 infants during delivery, according to an official study into the NHS’s greatest maternity crisis.
As per the independent investigation, which is looking into more than 1,860 instances of bad treatment, the Shropshire trust has failed to adequately investigate allegations of poor care by its personnel over decades.

Due to a major cultural preference to avoid cesarean sections, some women were given medication and made to endure painful forceps births that resulted in kids with crushed skulls as well as fractured bones.
There have been more than 40 infant fatalities and more than 50 infants with brain damage reported in a leaked study by The Independent last year. However, the number of parents reporting about subpar treatment has more than quadrupled since then.
“These included a number of maternal and baby deaths and many cases where babies suffered brain damage. “Families have told us of their experiences of pregnancies ending with stillbirth, newborn brain damage and the deaths of both babies and mothers. These families have shared with us their accounts of the overwhelming pain and sadness that never leaves them.”
What do we know so far?
England’s Health Secretary Jeremy Hunt announced an official inquiry in 2017 following 23 instances of suspected maternal errors were brought to the notice of the United Kingdom Government, investigating a “cluster” of avoidable and preterm newborn deaths throughout the two Healthcare institutions in the issue.
A little more than a year later, the details of the case were broadened to include 40 instances from 1998 to 2017, and then to 100. The number of incidents in issue now stands at over 2,000, dating back to 1979.
There have been several reports of newborns dying because of a lack of effective monitoring of fetal pulse rate and of late deliveries that led to a high number of fatalities.

After delivering stillborn babies at the Royal Shrewsbury Medical in 2014, mother-to-be Kelly Jones alleged that she was repeatedly disregarded by hospital staff who were aware of her agony throughout her pregnancy. Her story is among the most significant ones of the inquiry. As a result of a “delay in noticing the worsening in the fetal cardiac tracing as well as the lost opportunity for early delivery,” the trust linked their fatalities to oxygen deprivation in their brains.
The same thing happened to Rhiannon Davies in 2009 when medical officials failed to notice many potentially life-threatening problems and she tragically lost her six-hour-old baby.
“There can be no more complacency. There is a deep seated problem in maternity, a deeper seated problem in midwifery and a toxic issue at the heart of Shrewsbury’s specific midwifery and obstetric services. It’s about the mothers and their babies. And too many of them are coming to harm in your care.
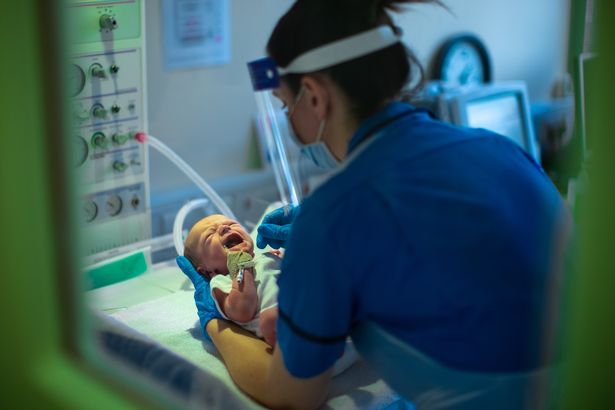
Among the findings of the Ockenden, the investigation would be that the institution had a subculture in which females were denied the opportunity to choose their labor preferences, as well as significant staffing problems.